Diet And Nutrition After Haemodialysis
June 4, 2021 | by Yashaswi Pathakamuri | Posted in Diseases, health, Nutrition Facts
Haemodialysis is the most common type of dialysis and the one most people are aware of. During the procedure, a tube is attached to a needle in your arm. Blood passes along the tube and into an external machine that filters it, before it’s passed back into the arm along another tube.
In hemodialysis, blood is removed from the body and filtered through a man-made membrane called a dialyzer, or artificial kidney, and then the filtered blood is returned to the body. The average person has about 10 to 12 pints of blood during dialysis only one pint (about two cups) is outside of the body at a time. Blood passes along the tube and into an external machine that filters it, before it’s passed back into the arm along another tube.
How is Haemodialysis done?
A blood vessel with a rapid flow of blood that is also close to the skin is needed for haemodialysis. This doesn’t exist naturally which is why an access has to be made. It is made during a short surgery using one of the two methods as shown below:
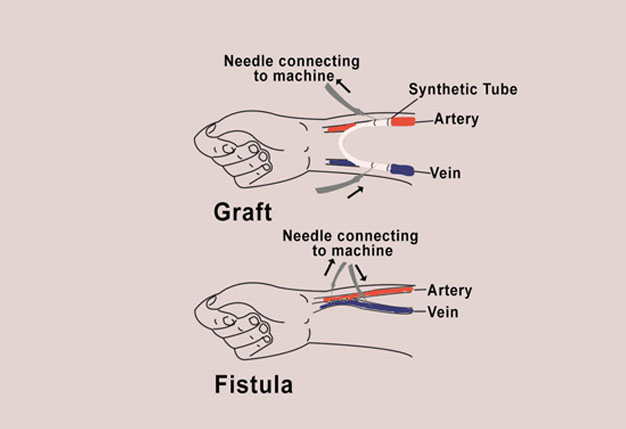
A fistula is made by connecting a vein to a nearby artery. Blood flows rapidly into the vein making it larger. It takes weeks to months before a fistula is ready for use.
A graft may be sewn between the artery and vein. Blood flows rapidly through the graft from the artery to vein. A graft is usually ready to be used during treatment after a week or two.
A plastic tube is attached to the needles connects the patient to the artificial kidney. Artificial kidney contains, two compartments, one for the patient’s blood and one for a cleaning solution called dialysate. A thin porous membrane separates these components.
Blood cells, proteins and other substances in blood remain in their compartment because they are large to pass through while smaller waste products like urea and creatinine in the blood and excess water pass through the holes of the membranes and are washed away. The clean blood now enters the patient’s body. Needed substances like calcium or dextrose can be added to dialysate.
Your hemodialysis care team monitors your treatment to make sure you’re getting the right amount of hemodialysis to remove enough wastes from your blood. Your weight and blood pressure are monitored very closely before, during and after your treatment.
Intervals of Haemodialysis
- Haemodialysis is done approximately 3-4 hours and is usually three times a week.
- Blood flow rates of 200-300 ml per minute are usual. Heparin is given intermittently or infused continuously to prevent clotting of blood in the dialyser during the usually 3 to 6 hours procedure.
- Adequate clearances can usually be achieved by a total of 12 hours of haemodialysis per week on thrice-weekly schedule.
Diet In Haemodialysis
Haemodialysis patients are unable to take oral supplements, inter-dialytic parenteral nutrition is given, which is a means of providing adernate calories and proteins. It is said that the patient on hemodialysis should eat high-quality protein because it produces less waste for removal during dialysis. High-quality protein comes from meat, poultry, fish, and eggs providing all the essential amino acids your body needs. Avoid processed meats such as hot dogs and canned chili, which have high amounts of sodium and phosphorus.
Patients on haemodialysis lose about 8-9 g of amino acids along with 2-3 g of peptides during each session, leading to a net loss of 10-13 g per dialysis.
The energy requirement of a haemodialysis patient is about 35 kcal/kg body weight and protein requirement is 1.1 g/kg for CAPD/CCPD patients, the protein requirement is 1.3 g/kg.
Dietary salt, potassium, phosphorus and water intake should be restricted to: salt 3-4 g; potassium 50-70 mEq/day, phosphorus 1g/day and water according to the urine out of the patient. Vitamin A is increased in dialysis patients and supplementation is not recommended.
Patients approaching final stage of renal disease but not yet initiated on haemodialysis should consume protein at the amount of 0.6 g/kg. If protein is restricted to a lower level, the diet should be supplemented with keto analogues of essential amino acids to prevent malnutrition.
Patients on chronic haemodialysis usually require a slightly reduced protein intake 0.8 to 1.0 g/kg, but a more stringent control of salt and potassium intake is needed to maintain satisfactory levels of blood urea nitrogen, potassium and blood pressure.
Certain fruits, vegetables, dairy products and other foods that are high in potassium will need to be restricted from your diet.
Foods To Avoid/Limit
- Foods with phosphate additives
- Chocolates
- Nuts
- Banana
- Salty meat
- Avocados
- Canned foods
- Dairy products
- Whole wheat bread
- Brown rice
- Oranges and orange juice.
How does the hemodialysis diet help?

The diet will include a balance of nutrients to help keep your body healthy and strong, while allowing the amount of potassium, phosphorus and sodium can be safely handled by your body.
Phosphorus is difficult for hemodialysis to filter from the blood so it’s important to limit foods that contain the mineral. Phosphorus can build to high levels in the bloodstream and cause weak bones, heart problems, joint pains.
Sodium makes your body to hold onto more fluid and raises your blood pressure. Eating less sodium and drinking less fluid can help you feel comfortable before and after your dialysis sessions.
Potassium is easily removed by dialysis, but when it builds up in the blood between treatments, it can cause muscle weakness and make your heart stop beating.
Fluid Intake In Haemodialysis
Too much intake of fluids between hemodialysis sessions can cause discomfort, including swelling, shortness of breath or high blood pressure. Fluid intake is not limited to what you can drink, it’s also hidden in some foods you eat, including gelatin, ice, watermelon, sauces and gravies. Your doctor or dietitian will help you learn the right amount
of fluid to drink each day.
Overall
- If you had dialysis, reduce your potassium, phosphorus, and sodium intake. It can be an important aspect of managing the disease.
- The high sodium, high potassium, and high phosphorus foods listed above are likely best limited or avoided.
- Dietary restrictions and nutrient intake recommendations will vary.
- Following a diet can seem daunting and a bit restrictive at times.
- If you had dialysis, reduce your potassium, phosphorus, and sodium intake. It can be an important aspect of managing the disease.
- The high sodium, high potassium, and high phosphorus foods listed above are likely best limited or avoided.
- Dietary restrictions and nutrient intake recommendations will vary.
- Following a diet can seem daunting and a bit restrictive at times.
- Certain fruits, vegetables, dairy products and other foods that are high in potassium will need to be restricted from your diet.